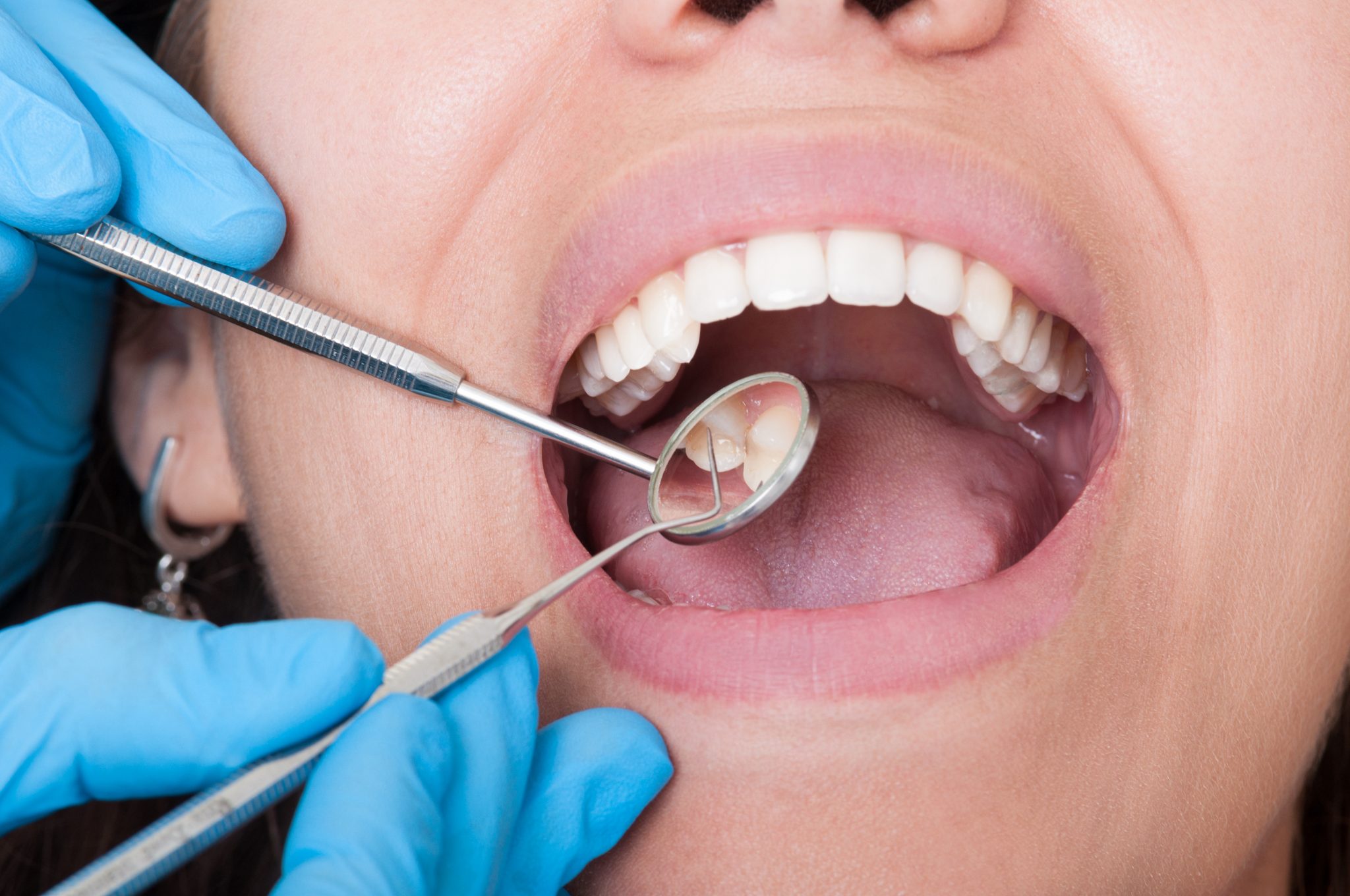
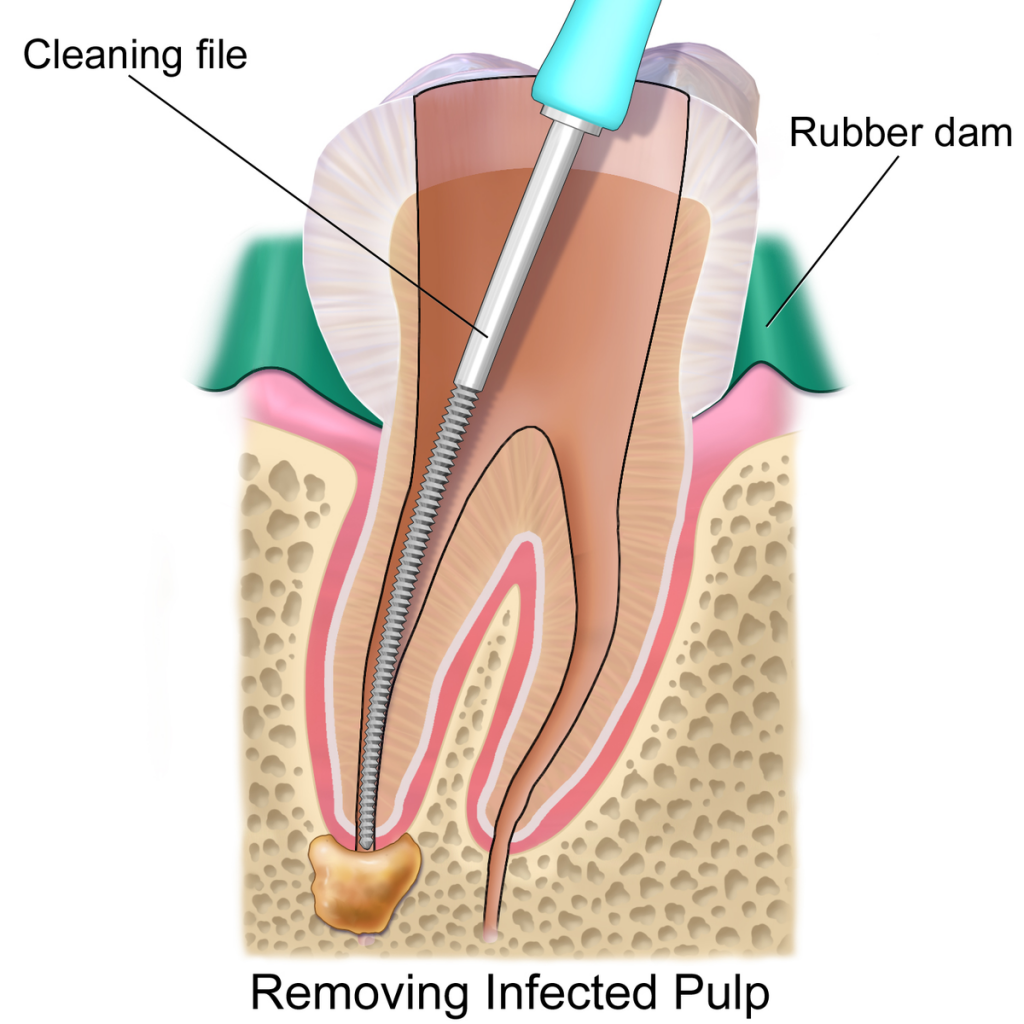
one of the many branches of dentistry is periodontics. Here are some signs that clearly indicate that you need to visit a periodontist immediately. Dentistry is a wide field that encompasses several different branches such as orthodontics, endodontics, prosthodontics, pediatrics, oral and maxillofacial, oral pathology, and periodontics. Four years of dental school qualifies an individual to practice general dentistry. For specialization, a general dentist has to undergo additional years of education and training.
Like all other dental specializations, a periodontist must undergo special training and education in the field. These individuals have the expertise and experience in treating gum-related problems and diseases. They not only have the expertise to diagnose periodontal diseases, but they have the knowledge and experience to treat these diseases
Periodontists provide treatment to patients that are in need of high-quality care due to severe gum diseases or complicated medical history. A general dentist may advise a patient to visit a periodontist when they need treatments such as scaling, root planing, or root surface debridement. Here are some signs that indicate that you need to see a periodontist right away! If you experience any of the following signs, you need to visit a periodontist immediately!
Swollen and Bleeding Gums
The most obvious signs that your gums are in bad shape is that they begin to swell, bleed, and appear red. When your gums bleed when you brush your teeth or floss, it is an indication that your gums need treatment. By visiting a periodontist, you can address a severe gum problem way before it gets serious.

Pain and Discomfort while Chewing
Pain and discomfort in your teeth are traceable. You can point to the exact the tooth that is causing the pain. However, if you experience pain while chewing within, around, or underneath your gums, you need to visit a periodontist.

Changes in Bites
Experience any changes in your bites? If your teeth begin to feel different while chewing, brushing, or talking, it is a sign that you are falling victim to a periodontal problem. Leaving this unaddressed for long can turn the minor issues into serious and long-term periodontal problems.
Chronic Bad Breath
Persistent bad breath even after extensive oral care indicates that
there is a problem in your gums. It is one of the first signs of gum disease. If you are experiencing a similar situation, make sure you schedule an appointment with a periodontist.
Teeth Begin to Feel Loose
Loose teeth might not be such a big issue for a baby and a young kid, but for an adult, it is a serious concern. If any of your teeth begin to feel loose, visit a periodontist without giving the idea any second thoughts. The sooner you realize you need a periodontist, the better it is for your gums. They can help in a timely diagnosis of gum diseases and addressing the problems before they become serious!